Pre-Authorization
We obtain patient information to secure prior authorization for inpatient and outpatient procedures, as well as hospital admission pre-certifications, to help you save time and get maximum reimbursements.


added on the EMR


of the patient are found




documents



Why Choose Us
Reduced claim denials
Ineffective pre-authorization processes can lead to increased claim denials, resulting in additional effort on rework. By reducing the prior authorization-related denials, we ensure that the total number of claim denials is reduced and the cash flow is accelerated.
Improved patient satisfaction
By following a streamlined authorization process, patients can be scheduled with the physicians for care reviews in a timely manner, improving speed to care delivery.
Healthcare providers can focus on delivering premium care
As Sypore takes over the entire process of pre-authorization at less than one-third of the cost, healthcare providers can now utilize their undivided attention to deliver premium care to patients.
Ready To Talk?
Learn how we transform the revenue cycle with solutions that streamline the patient experience, drive operational efficiency, and improve financial performance.
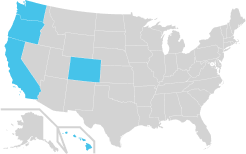
The Western States
- Colorado
- California
- Oregon
- Washington
- Hawaii
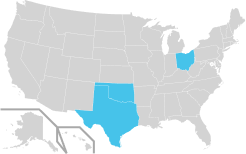
The Central States
- Texas
- Oklahoma
- Ohio
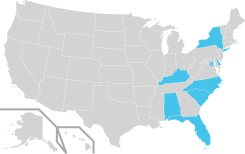
The Eastern States
- Alabama
- Delaware
- Florida
- Kentucky
- New York
- South Carolina
- North Carolina
- DC